Ticks and parasites: how, when and why... how to remove them without doing harm
Practical advice from the clinic
With the arrival of the mild season, the spectre of tick infestation recurs relentlessly for dog and cat owners. This happens even if many of them are properly informed by their veterinary doctors or have clearly understood by now the concept of global warming and its significance in the parasitological field.
In this sense, with winters no longer being particularly harsh, especially in the areas further south of the Peninsula, as well as applying a constant parasite treatment with specific products on the animal and in the environment; it would be a good idea, when returning from every walk with your dog, to inspect its body not only visually, but by stroking it and moving your fingers between the hairs of its coat, until you get to the skin (like when we shampoo our hair) to look for any suspicious "growths". Your inspection should be done without neglecting to check the interdigital webbing between its toes and moving around its paw pads, the contour of its eyes, its ears and the area around the anal sphincter. On the other hand, the animals cannot sense ticks on their own body due to cushioning structures on the extremities of parasite limbs, making movement imperceptible, which is why the animals do not warn us with outward signs of discomfort.
This precautionary inspection, if carried out with delicacy and patience, can also become a very rewarding and pleasant ritual for the animal and its resulting feeling of wellness will undoubtedly strengthen the owner-pet relationship!

What is a tick, and why do we need to pay so much attention to it?
Ticks are arthropods belonging to the Class Arachnida (suborder IXODIDA), and are mites capable of parasitizing various animal species and even humans. They are of socio-sanitary importance because, feeding on the blood of their hosts, they can transmit different viral (e.g., tick encephalitis), protozoans (e.g., Piroplasmosis, Hepatozoonosis), and bacterial (e.g., Borreliosis, Anaplasmosis, Ehrlichiosis, Rickettsiosis) diseases.
In addition, in the case of a massive and chronic tick infestation, anemia may develop in puppies and animals of fragile health.
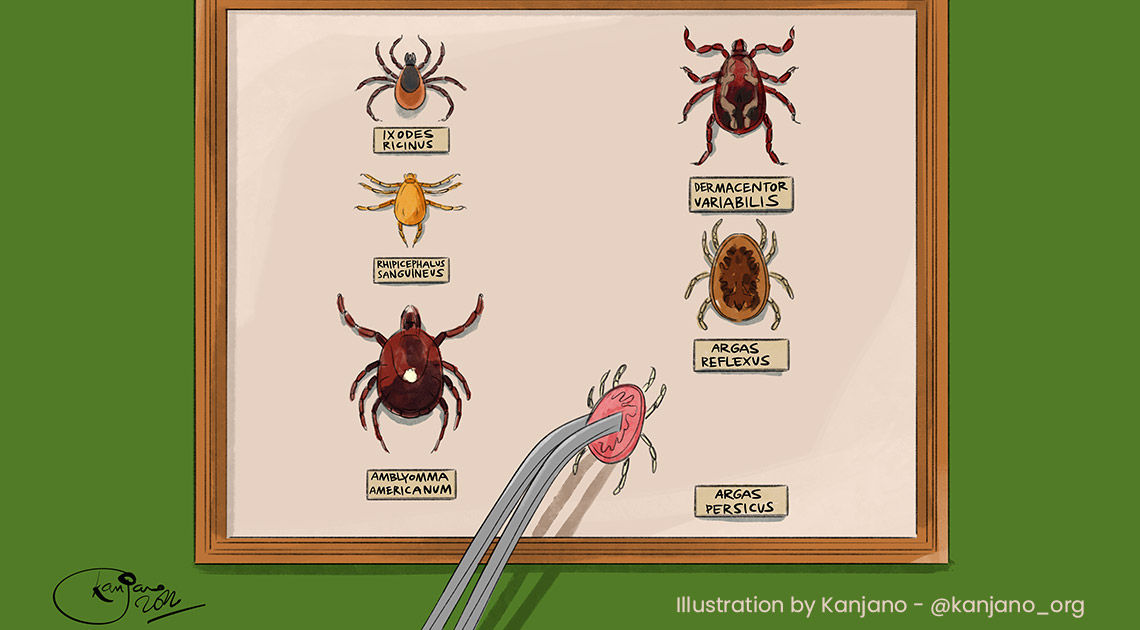
The most common species is the Ixodes ricinus (the so called "castor bean tick", the most reported in cases of human tick bites) and Rhipicephalus sanguineous (typical dog tick but which, in the absence of its preferential host, can also parasitize humans and, more rarely, cats).
Their body is oval and of a brownish color, but they can vary both in volume (from a few millimetres to more than a centimetre) and in colour (from reddish brown to light brown-beige), depending on their stage of development and blood intake. Its life cycle is divided into stages, which occur partly on the host and partly in the environment and it is for this reason that a combined animal-environment pest strategy should be implemented to fight against the parasite effectively.
Ticks are present not only in rural environments sheltered from the intense cold and with a high density of animals (kennels, stables, barns), but also in peri-urban and urban areas where dogs transit and there are nooks and crannies suitable for the parasite's conservation and development stages (parks, gardens and uncultivated areas, cracks in walls and pavements, edges of roads and steps, gardens and private and communal gardens, brushwood).
In the event of not finding a host and favorable environmental conditions, ticks can enter a state of temporary quiescence and resist for long periods of time to absolute fasting.
The rapid removal of the tick has a threefold advantage:
- To stop local irritation from the parasite bite and from the secretion of substances through the saliva that have the task of sealing its buccal apparatus to the host's skin, preventing the coagulation of blood during sucking;
- To prevent the tick from detaching from the host after its blood meal and colonising the environment and thus from possible transmition of any pathogens to other subjects;
 The general question animal owners ask me when they visit my clinic is: "so, if I have treated my animal with antiparasitic medicine, then why does it have ticks?"
The general question animal owners ask me when they visit my clinic is: "so, if I have treated my animal with antiparasitic medicine, then why does it have ticks?"
The answer is multiple:
- a not punctual administration, so the pesticide no longer performs its full function;
- an incorrect application (wide pet collars make it difficult to spread the active substance properly on the body surface );
- when a spot-on antiparasitic is applied on the hair and not the skin;
- when the animal vomits not long after taking an oral antiparasitic;
- Baths with detergents not long after spot-on pesticide applications; or walks after a detergent bath immediately after the reapplication of an antiparasitic collar that, therefore, has not yet been able to reactivate the animal's protective "barrier";
- Poor efficacy of the active substance of the antiparasitic leading to less sensitivity of ticks present in the frequented environment (environmental resistance);
- Pesticide treatment carried out only on the animal when faced with massive environment infestation (own garden or areas frequented by the dog).
How to remove a tick?
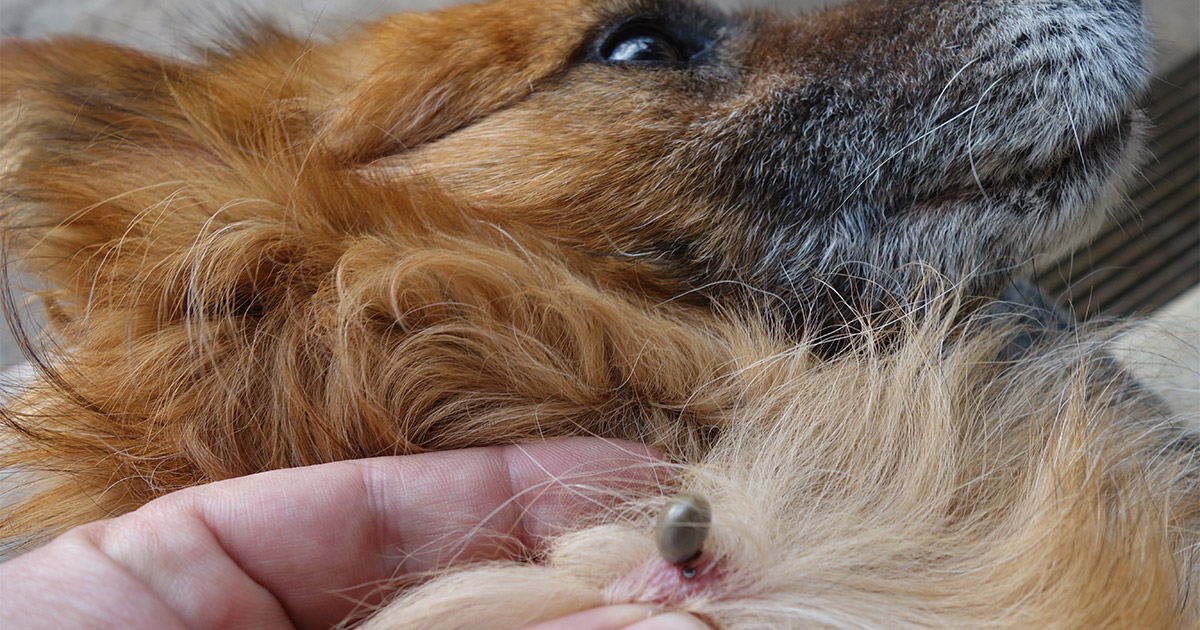
Bearing in mind the rostral apparatus with which the tick enters the skin, grab the tick with a pair of eyebrow tweezers or a dedicated hook available in specialized shops, holding it close to the skin so as not to risk crushing the tick's body (If you do not have a suitable instrument, you can use your thumb and index finger, protected by a latex glove to prevent the transmission of infections if you have micro skin lesions).

Care should be taken not to compress the body of the parasite since the transmission of pathogens occurs in the regurgitation stages; for the same reason, do not use alcohol, gasoline, acetone, triline, ammonia, oil or fat in the "legendary" attempt to "suffocate" or "stun" the tick and encourage detachment. In fact, the tick breathes very slowly (only a few breaths per hour), so we would not only fail in our attempt but could favor salivation and regurgitation by "disturbing" it, with the consequences described above, as well as further irritating the parasite attachment site where a small, continuous rupture of the skin has been created.
Once the head is grasped, a delicate traction must be exerted, with a small rotation movement to avoid the oral apparatus of the tick from remaining stuck, which could lead to the growth of granulomas or abscesses. Once the tick has been removed, disinfect the affected skin area.
If, after a few days, a suspicious redness or local swelling appears at the point of removal, you should consult a veterinary doctor.

The removed tick must be eliminated, for example by burning it after wrapping it in a piece of paper, in order to prevent it from returning to its initial host - or to a new one, or infesting the environment by spreading the eggs it carries.
Sometimes pet owners are not sure that what they have removed from their dog’s body is a tick or, conversely, harbor the doubt that the growth they see may not be a small skin formation but, rather, the dreaded parasite. In the first case, it is advisable to keep "the body of the crime" in a closed container containing alcohol and show it to a veterinarian; in the second, avoid pulling at it so as not to traumatize any small skin formations that should be looked at and investigated.
Many times in my outpatient experience, I have found myself in the presence of pet owners worried about a tick that, on close inspection, turned out to be a small nipple on a male dog!
Dott.ssa Alessandra Di Marzio. Independent Veterinary Physician.